|
Getting your Trinity Audio player ready...
|
The research by global healthcare company, Sunstar, analyzed the relationships among blood markers, oral indicators and oral hygiene habits based on medical records of 145 patients with type 2 diabetes from the Sunstar Foundation’s Senri Dental Clinic in Japan. It found that even with reduced plaque in patients, higher HbA1C and high-sensitivity CRP (C-reactive protein) levels were associated with increased gum bleeding in patients with type 2 diabetes.
The study, ‘Management of periodontal disease based on diabetes-related blood markers,’ recently presented at a meeting of the Japan Diabetes Society, showed that while plaque control is fundamental in preventing gum bleeding, patients with high blood markers of HbA1c and high-sensitivity CRP had higher gum bleeding rates, even when their plaque control was as good as those with lower blood markers.
The frequency of oral hygiene habits, such as interdental cleaning and rinsing with oral care products, as well as toothbrushing, were also associated with good plaque control.
Following the research, Senri Dental Clinic has now introduced personalized plaque control routines and targets for periodontal patients with diabetes and is providing individual oral hygiene guidance to achieve these goals.
The authors are similarly advising dental professionals to incorporate blood-marker targets (e.g. HbA1c and CRP) in patients with type 2 diabetes and recommending collaborative management between oral health professionals and medical providers in patients with type 2 diabetes, rather than one-off referrals.
While the bidirectional link between diabetes and periodontal disease is well established, with the Japanese Clinical Practice Guideline for Diabetes recommending periodontal treatment for patients with type 2 diabetes for effective glycemic control, most existing studies have focused on the initial treatment of periodontal disease. There has been little focus on the need for, or approaches to, ongoing oral health management based on blood markers.
The full study
This study aimed to clarify the relationship between blood markers, periodontal indicators and oral hygiene habits in people with type 2 diabetes receiving treatment or ongoing periodontal care.
Blood markers and gum bleeding: Multivariate analysis considering plaque amount
In addition to the plaque amount, the contribution of systemic factors (measured using the blood markers HbA1c and high-sensitivity CRP) to the gingival bleeding rate were examined using a generalized linear model.
In Models 1 and 2, higher HbA1c and high-sensitivity CRP were each independently associated with increased gum bleeding, even after adjusting for plaque levels. When both markers were combined (Model 3), their individual significance disappeared, suggesting interplay between glycemic control and systemic inflammation. In Model 4, all factors were significant indicating that poor glycemic control and elevated systemic inflammation combined lead to a stronger gum bleeding response.
Detailed research findings
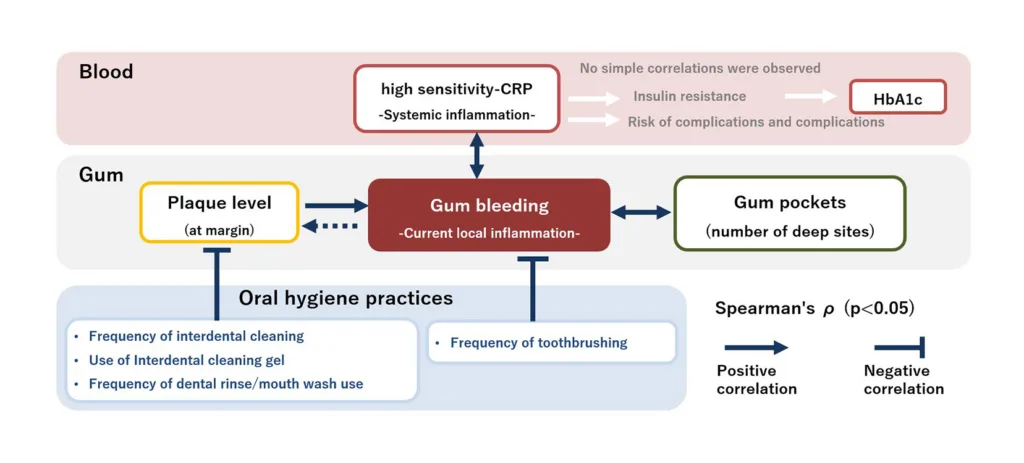
The gingival bleeding rate was associated with high-sensitivity CRP, other oral indicators and toothbrushing frequency, suggesting that the gingival bleeding rate serves as an important indicator connecting these factors.
Oral hygiene habits such as interdental cleaning and rinsing with oral care products in addition to toothbrushing were also shown to correlate with lower plaque levels.
 Sunstar Suisse SA
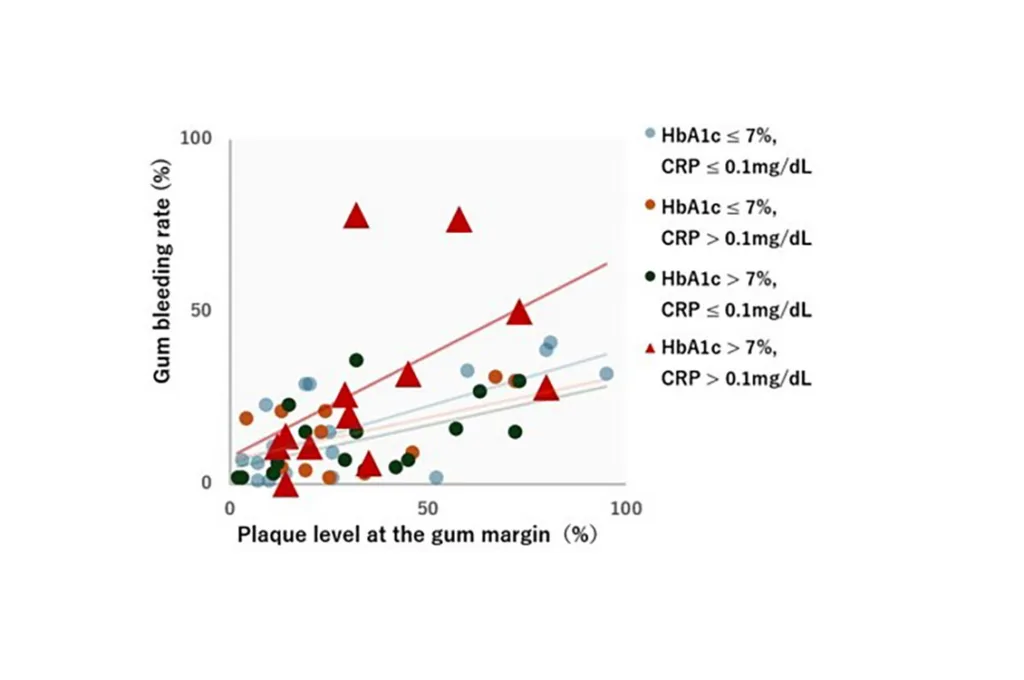
Sunstar Suisse SARelationship between plaque level and gum bleeding by blood marker combinations
Participants were grouped using HbA1c of 7% and high-sensitivity CRP of 0.1 mg/dL thresholds:
- HbA1c ≤ 7%, CRP ≤ 0.1mg/dL
- HbA1c ≤ 7%, CRP > 0.1mg/dL
- HbA1c > 7%, CRP ≤ 0.1mg/dL
- HbA1c > 7%, CRP > 0.1mg/dL
In all four groups, an increase in plaque amount was associated with a higher bleeding rate, with the rate particularly high in the group with both high HbA1c and high CRP. This shows that in those patients with even the same amount of plaque, those with high blood sugar and systemic inflammation have a higher bleeding rate.
 Sunstar Suisse SA
Sunstar Suisse SAThese results suggest that systemic factors affect gum bleeding even in the stable and maintenance phases of periodontal disease. Senri Dental Clinic is now using a risk assessment for patients with type 2 diabetes based on blood test values and setting individual plaque control goals for its patients. The clinic also provides self-care oral hygiene to help patients achieve the next plaque control goal.
Dr. Hidenori Suzuki, Director, Sunstar Foundation Senri Dental Clinic, commented: “For patients with both periodontal disease and diabetes, we’ve always explained the importance of plaque control and the relationship between the two diseases, but previously it has been difficult to present concrete goals.
“Although this is a cross-sectional study based on a single dental practice, we’re now able to quantify plaque control goals based on blood markers.
“Periodontal treatment often takes a long time and some patients can feel anxious thinking ‚when will it end?‘ or ‚is it effective?‘. Sharing personalized goals between patients and their care providers is the first step toward motivating both parties to work together on long-term treatment.“
Research method
An analytical cross-sectional study using existing clinical records, medical and interview data from patients with self-reported type 2 diabetes who received stable-phase supportive periodontal therapy (SPT) or maintenance care from the Senri Dental Clinic between September 2021 and January 2024.
Analysis included background: Gender, age, presence of regular internal‑medicine care, insulin use, BMI, smoking. Blood markers: HbA1c, high-sensitivity CRP. Oral indicators: periodontal pocket sites (≥4 mm), plaque levels, gum bleeding rate and oral hygiene habits: brushing frequency, interdental cleaning, mouth rinsing and use of interdental gel.
Quelle: Sunstar Suisse SA
 Entdecke CME Artikel
Entdecke CME Artikel  Entdecke Artikel mit Download
Entdecke Artikel mit Download 



 Mit Google einloggen
Mit Google einloggen
 Mit Facebook einloggen
Mit Facebook einloggen
Keine Kommentare.